Luteal Phase: Symptoms, Causes, And Hormones
Did you know that your menstrual cycle is divided into two phases? This fact is surprising yet essential information whether or not you’re trying to conceive.

The luteal phase of your menstrual cycle immediately follows ovulation. Below you’ll learn all about:
- Exactly what this phase is.
- When it is and how long it lasts.
- Hormonal changes that occur.
- How it affects fertility.
You’ll also find tips on monitoring your luteal phase. Read on to discover everything you need to know about this crucial part of your menstrual cycle.
What Is The Luteal Phase?
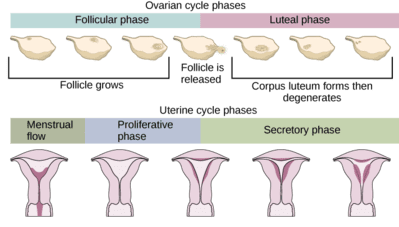
The luteal phase is the post-ovulation phase of your menstrual cycle. The pre-ovulation phase of your ovarian cycle is the follicular phase.
The follicular phase is when follicles and develop in the fallopian tubes. Follicle development prepares an egg for ovulation.
After ovulation, the luteal phase starts. The follicle that contains the egg from the follicular phase turns into something called the corpus luteum. When the corpus luteum grows, your progesterone levels rise.
Progesterone peaks halfway through the luteal phase. The corpus luteum dissolves if there is no fertilized egg or implantation. This causes progesterone levels to drop (learn more on your period and progesterone here).
The luteal phase ends when your period begins. The first day of your period is the first day of the follicular phase, and the cycle starts over again.
How Long Is The Luteal Phase?
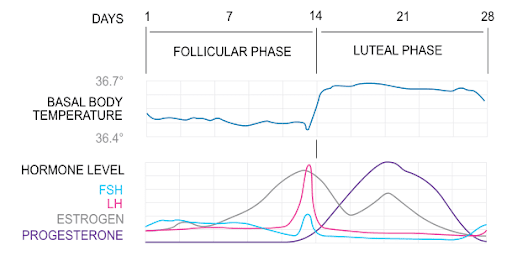
The average luteal phase is 12 to 14 days long, but it can last 10 to 17 days. You’ll often read that 14 days is normal. This standard is based on a 28-day cycle, but menstrual cycles vary greatly.
Some medical sources say cycles may last 21 to 35 days long. Others state 21 to 45 days is normal. This makes it hard to know how long your luteal phase is and when the phase occurs.
You can determine phase length by tracking your cycle or by using a luteal phase calculator. Count the days between ovulation and the first day of your period. That is how long your luteal phase is. Some tracking methods are:
- Basal body temperature (BBT) charting
- Ovulation calculators/calendars
- Checking cervical mucus
- Ovulation prediction kits (OPKs)
OPKs detect luteinizing hormones, and this makes them more accurate than other methods. However, the average OPK doesn’t offer personalized information. They simply use a threshold to detect LH to estimate if you’re ovulating.
To correctly track your cycle and luteal phase, you need personalized feedback. The Mira analyzer is part of Mira’s advanced fertility tracking kit and measures LH levels in mIU/mL. This lets you see your exact hormone levels.
The automatic charting and AI-powered cycle personalization show your LH levels and surges. You can monitor peaks, declines, and menstruation through the app to detect your luteal phase.
Why Is It Important To Know Your Luteal Phase?
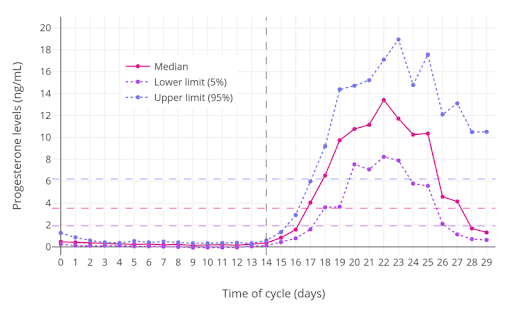
Knowing as much as possible about your menstrual cycle is essential. The chart above shows different hormone levels throughout your cycle.
Progesterone is crucial for the luteal phase. For women trying to conceive (TTC), it’s important to know about progesterone levels because:
- Progesterone from the luteal phase thickens the lining of the uterus.
- Thick lining is needed for implantation.
- Short luteal phases (less than ten days) may indicate low progesterone levels.
- Low progesterone levels can prevent conception.
Women who aren’t TTC should also learn about this phase. Low progesterone levels create an unhealthy hormonal imbalance. When estrogen and progesterone are unbalanced, women may experience:
- Fibroids
- Decreased libido
- Fibrocystic breast disease
- Weight gain
- Mood swings
- Depression
While you cannot track progesterone levels without a physician, you can monitor LH levels by tracking fertility hormones at home. If you notice your luteal phases are less than ten days, make an appointment with your OBGYN to check your progesterone levels.
What Are the Luteal Phase Signs And Symptoms?

When progesterone levels drop during the luteal phase, some women experience physical and mental symptoms. These issues are better known as premenstrual syndrome (PMS) symptoms and include:
- headaches
- bloating
- mood swings
- acne
- appetite changes
- fatigue
- insomnia
- nausea
- muscle pain
- abdominal cramps
These symptoms are mild for some women and severe for others. There are over-the-counter and prescription treatments for different symptoms.
- Nonsteroidal anti-inflammatory drugs (NSAIDs) – NSAIDs are over-the-counter pain relievers like ibuprofen and acetaminophen. They are used to relieve headaches and cramps.
- Diuretics – Diuretics are also known as water pills, and they relieve bloating. Over-the-counter PMS medications like Midol and Pamprin combine NSAIDs and diuretics.
- Oral contraceptives – Birth control pills contain hormones that release steadily into the bloodstream. These hormones treat symptoms like cramps, acne, and mood swings.
- Antidepressants – Some women experience severe PMS and are diagnosed with premenstrual dysphoric disorder (PMDD). Antidepressants can relieve anxiety, depression, and mood swings from PMDD.
If you’re not sure how to treat luteal phase side effects, ask your doctor which options are best for your symptoms.
What Is A Luteal Phase Defect?
A luteal phase deficiency or defect is when uterine lining doesn’t thicken properly. It’s a potential fertility problem because an egg cannot implant if the lining isn’t thick enough. This can happen if:
- Ovaries do not produce enough progesterone (short luteal phase).
- The uterine lining does not respond to progesterone.
There are several health issues linked to luteal phase defects. These medical conditions can affect progesterone and other reproductive hormones.
- Endometriosis
- Polycystic ovary syndrome (PCOS)
- Obesity
- Anorexia
- Hyperprolactinemia
- Thyroid disorders
When these problems are treated, luteal phase defects may also be corrected. Treatment is based on a woman’s health needs, and some may not require any treatment.
Women who want to get pregnant need treatment to correct hormone imbalances. Methods of treatment include:
- Human chorionic gonadotropin (hCG) – hCG, AKA the pregnancy hormone, can help with ovulation and producing progesterone.
- Clomiphene citrate – This medication, known as Clomid, is used to treat infertile women. It stimulates hormone increases to help growth and release of eggs.
- Progesterone – This hormone is available in the form of pills, injections, and suppositories.
Treatment can also include lifestyle changes. Our blog post about boosting fertility naturally features great examples of positive changes to make.
Track Your Cycle And Take Charge
To take charge of your health, track your luteal phase and the rest of your cycle. When tracking your cycle, you can monitor hormone levels, note patterns, and spot changes. If you notice any sudden irregularities or symptoms, get advice from your OBGYN to resolve any problems.

Mira’s Editorial Process
All content produced by Mira meets stringent editorial standards, ensuring excellence and accuracy in language and medical precision. Every piece undergoes thorough fact-checking and review by qualified professionals. Check out our full editorial process to learn more.










